Tin and Iodine
| Cellular Nutrition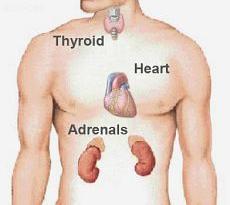
Tin (Sn) and Iodine (I) are associated trace elements considered essential to human health, although there is controversy among some researchers regarding the essentiality of tin, and its value in human nutrition.
Tin is associated with iodine the same way as calcium is associated with magnesium, with tin supporting the Adrenals, and iodine supporting the Thyroid. Both, adrenals and the thyroid affect cardiac functions, so low or high levels of tin and iodine can subsequently affect cardiac functions as well, whereby tin / adrenals have some controlling effect on the left cardiac output, and iodine / thyroid have some controlling effect on the right cardiac output.
Outside of heart disease (and diseases of heart-supporting organs), left-sided cardiac insufficiency may result secondary to low adrenals, which in turn may be due to low tin (or other adrenal-supporting nutrients). Right-sided cardiac insufficiency may result secondary to low thyroid, which in turn may be due to low iodine (or other thyroid-supporting nutrients).
In addition to tin and iodine, a number of other nutritional factors either directly or indirectly affect the thyroid and adrenals, and subsequently cardiac functions, which include nickel, cobalt, zinc, potassium, manganese, iron, bismuth, lithium, most B-vitamins..., and the amino acid tyrosine, which in combination with iodine is manufactured into the thyroid hormone thyroxine (T4), while selenium affects T4 to T3 (triiodothyronine) conversion.
Fatigue and/or depression are common with Cardiac Insufficiency of either side, however symptoms of insufficiency specific to the left side are generally more often breathing difficulties or asthma, and symptoms specific to the right side are more commonly experienced as edema, particularly swelling of hands and feet.
To prevent deficiency, iodine had been routinely added to baked goods, until it was eventually replaced with bromine in the 1960s. Unfortunately, bromine competes with iodine, and by affecting its uptake by the thyroid gland results in progressive iodine deficiency, which eventually leads to hypothyroidism.
Potential symptoms with diminished thyroid functions include physical and mental fatigue, depression, mood swings, sleep disturbances, memory problems, asthma, heart palpitations, sweating, dry skin, brittle hair and nails, PMS, reduced libido, menstrual problems, post-nasal drip and frequent sinus infections, cold hands and feet, constipation, ADHD, flatulence, obesity, fluid retention, plus greater risk for fibrocystic breast disease, and in addition to thyroid cancer, various estrogen-positive cancers (breast, uterine, ovarian, prostate...).
In Canada and the US, Iodine Deficiency has not been "officially" recognized since the introduction of iodized table salt, however for various reasons - one of them being that some people just don't use any table salt - a large percentage of the population benefits from supplementing iodine in addition to whatever amounts they get from dietary sources. In fact, most individuals who are routinely put on medications for hypothyroid conditions could normalize their thyroid by simply supplementing extra iodine (and/or perhaps L-tyrosine), instead of taking thyroid medications.
Vitamin B6 can be helpful for hypothyroidism when triggered by abnormal liver functions (which may be due to high estrogen, or long-term use of drugs such as Tylenol, lithium, alcohol, etc.), however the body seems to eventually adapt to whatever amounts are supplemented, so in order to maintain normal thyroid activity with Vitamin B6, ever-increasing amounts would have to be taken. This of course becomes self-limiting, since magnesium levels (raised by Vitamin B6 intake), and Vitamin B6 itself would become unreasonably high in the long run, and there is a potential risk of Vitamin B6 overdose-related toxic effects.

Ideally, thyroid and iodine levels should be measured, so the most appropriate therapy is implemented, and any hyperthyroid conditions are caught in time as well, which could otherwise lead to bone density, or heart problems. Since iodine levels, along with a host of other interactive trace elements such as fluoride, tin, nickel, cobalt, and many others are assessed at every patient consultation, Dr. Ronald Roth had monitored hundreds of individuals who have been ingesting as much as 5mg - 6mg of organically bound iodine (40x the RDA / RDI) for many years, without experiencing any ill effects, so toxicity - for most people - is not an issue, however out of thousands of other patients Dr. Ronald Roth had tested, the great majority required 1mg or less of iodine per day to maintain normal to optimal levels.
Some practitioners recommend a standard adult dose of 12.5mg of iodine daily, including for those suffering from Hashimoto’s thyroiditis, or Graves disease (Hyperthyroidism). It makes more sense though to adjust iodine levels to actual patient requirements - rather than using a standard trial and error dose since too much iodine can not only lead to Hyperthyroidism, but also Hypothyroidism (including goiter) in rare cases due to diminishing iodine uptake (binding) by the thyroid, following ongoing iodine overdose. This also applies during pregnancy, where too much - just like too little iodine - can adversely affect the baby. Supplementing normal (RDA / RDI) amounts of iodine following long-standing iodine deficiency can trigger hyperthyroidism in rare instances. At the same time, a high intake of goitrogenic / cruciferous vegetables may equally require a higher intake of iodine:
Goiter may not only develop following long-standing, inadequate iodine intake,[1] but also after consuming large amounts of goitrogenic food sources that interfere with iodine uptake and/or thyroid metabolism. These foods, also known as "goitrogens," include Brussels sprouts, sweet potatoes, lima beans, cauliflower, rutabaga, broccoli, cabbage, cassava, and nitrate-rich food sources. In some parts of the world, there are still cases emerging where children, as a result of ingesting large amounts of goitrogenic foods, end up with mental retardation, which could have been prevented with iodine supplementation. On a similar note, regular consumption of soy products - because of their phytoestrogenic properties - can also have a significant (depressing) impact on thyroid functions.
With Fibrocystic Breast Disease, sufficient iodine intake is an important consideration, as are adequate amounts of Vitamin E and essential fatty acids (EFAs), however, caffeine sources such as tea, coffee, cola drinks, cocoa / chocolate... should be avoided, or eliminated entirely.
For mild hyperthyroidism, PABA is usually helpful, and raising magnesium (if low) will at times help normalize a slightly overactive thyroid as well. Some premenopausal or postmenopausal women will, as a result of declining estrogen levels, become hyperthyroid. Most of these cases readily improve with estrogen therapy (i.e. estriol, phytoestrogens), or with supplementing manganese and/or PABA, both of which have estrogenic properties.
Although it is not an essential trace mineral, bromine is a fairly potent thyroid and iodine antagonist [2] that works well in humans and animals, and is indicated for more severe cases of hyperthyroidism.
Kelp - or other types of seaweed - are sometimes recommended as a source of iodine, however kelp also contains varying amounts of bromine, so its iodine / bromine ratio will ultimately determine whether it will have a beneficial or adverse effect on someone's thyroid. Some people develop an acne-like skin condition as a result of consuming iodine-containing foods, with the culprit being frequently bromine (which is usually present as well), but rarely iodine.
See Acu-Cell "Tin - Health Effects" for details and research results about the Trace Element Tin.
Using Potassium Iodide tablets to protect from Nuclear Fallout
In the event of a radioactive material fallout following a nuclear disaster at a power plant, or a terrorist attack, potassium iodide can to some extent protect the thyroid gland from developing cancer following exposure to the radioactive isotopes of iodine (Iodine 131, or radioiodine), however it does not protect from other radioactive material, such as contamination with plutonium, americium, or curium which can occur through inhalation, ingestion, or contact with open wounds as a result of industrial accidents, or from terrorist attacks using "dirty bombs." To increase the rate of elimination of these contaminants, the FDA (US) has approved the two drugs pentetate calcium trisodium (Ca-DTPA), and pentetate zinc trisodium (Zn-DTPA) via injection.
Normally, the thyroid gets the iodine necessary to produce thyroxine from dietary sources such as seaweed, seafood, shellfish, iodized salt, and some seeds and dairy, however after a nuclear fallout, large amounts of of radioactive iodine become available for uptake, with the thyroid being unable to distinguish between radioactive, and non-radioactive iodine. As a result, the thyroid will absorb and retain excessive amounts of radioiodine, with those suffering from hypothyroidism, or children, being adversely affected the most.

Fortunately, if enough potassium iodide (KI) or potassium Iodate (KIO3) are taken orally from 30 minutes (a couple of hours according to some sources), to a day before being exposed to radioactive iodine, then the thyroid is saturated enough to prevent radioactive iodine from being absorbed, and thus prevents the ensuing damage to the thyroid gland which would otherwise result.
The small amount (about 1%) of radioactive iodine that may still be absorbed is eliminated by the kidneys. The standard 130 mg potassium iodide tablets that are used for thyroid protection contain about 77% iodine, which is nearly 1000x the Recommended Dietary Intake, or Dietary Reference Intake of iodine.
Please note: Dietary sources of iodine do not provide sufficient iodine to saturate the thyroid enough to prevent radioactive iodine absorption. For instance, a teaspoon of iodized salt provides approximately 6 g of salt, which contains only about 520 mcg (micrograms) of potassium iodide, so a 130 mg (milligram) tablet of potassium iodide provides 250x more potassium iodide, while the use of sea salt would require 30x the amount of iodized salt, which would make potassium iodide tablets 7500x stronger than sea salt. The same applies to other dietary sources of iodine such as kelp, or seafood, where enormous amounts would have to be consumed to (theoretically only) achieve a thyroid-protective effect.
It should also be mentioned that elemental (free) iodine, or tincture of iodine (which can be poisonous) is not effective as a blocking agent to prevent thyroid damage, although there are claims that stronger solutions of topical applications would work, which however has not been officially verified.
Additional FDA Patient Information
Use of 130 mg Potassium Iodide USP tablets for thyroid blocking:
Take potassium iodide tablets only when Public Health officials tell you. In a Radiation Emergency, radioactive iodine could be released into the air. Potassium iodide (a form of iodine) can help protect you. If you are told to take this drug, take it one time every 24 hours. Do not take it more often. More will not help you and may increase the risk of side effects. You will likely be told not to take the drug for more than 10 days.
Warning:
Do not take Potassium Iodide if you know you are allergic to Iodine (see side effects below). Keep out of the reach of children. In case of overdose or allergic reaction, contact a physician or public health authority.
Indications:
Thyroid blocking in a radiation emergency only.
Dose (U.S.):
Adults and children one year of age or older: One 130 mg tablet once a day. Crush for small children. Babies under one year of age: One-half 130 mg tablet once a day. Crush first.
Dose (World Health Organisation):
| Adults: | One 130 mg tablet once a day |
| Children age 3-18: | One-half 130 mg tablet once a day (65 mg)* |
| Children under 3 years old: | One-quarter 130 mg tablet once a day (32 mg) |
| Babies under 1 month old: | One-eighth 130 mg tablet once a day (16 mg) |
* heavier / larger teens should use 130 mg (adult-size) tablets.
Take for 10 days unless directed otherwise by state or local public health authorities. Store at controlled room temperature between 15 to 30C (59 to 86 degrees F). Keep bottle tightly closed and protect from light.
You may take potassium iodide even if you are taking medicines for a thyroid problem (for example, a thyroid hormone or anti-thyroid drug). Pregnant and nursing women and babies and children may also take this drug.
Side effects:
Usually, side effects of potassium iodide happen when people take higher doses for a long time. You should be careful not to take more than the recommended dose or take it for longer than you are told. Side effects are unlikely because of the low dose and the short time you will be taking the drug. Possible side effects include skin rashes, swelling of the salivary glands, and "iodism" (metallic taste, burning mouth and throat, sore teeth and gums, symptoms of a head cold, and sometimes stomach upset and diarrhea).
A few people have an allergic reaction with more serious symptoms. These could be fever, joint pains, or swelling of parts of the face and body, and at times severe shortness of breath requiring immediate medical attention. Taking potassium iodide may rarely cause overactivity of the thyroid gland, underactivity of the thyroid gland, or enlargement of the thyroid gland (goiter).
What to do if side effects occur:
If the side effects are severe or if you have an allergic reaction, stop taking potassium iodide. Then, if possible, call a doctor or public health authority for instructions.

 Manganese may help with some symptoms of Parkinson's disease such as muscle rigidity and twitching...
Manganese may help with some symptoms of Parkinson's disease such as muscle rigidity and twitching...
 Research shows that phytosterols such as beta-sitosterol may help normalize the function of natural killer cells and T-helper lymphocytes...
Research shows that phytosterols such as beta-sitosterol may help normalize the function of natural killer cells and T-helper lymphocytes...
 Iron deficiency may be suspect with some forms of ADHD. 84% of children with ADHD were found to have abnormally low levels of ferritin...
Iron deficiency may be suspect with some forms of ADHD. 84% of children with ADHD were found to have abnormally low levels of ferritin...
 A high intake of B Vitamins can trigger heart palpitations, HBP, major complications in patients with congestive heart disease...
A high intake of B Vitamins can trigger heart palpitations, HBP, major complications in patients with congestive heart disease...